Case Studies of Patients With HS
CASE STUDY 1:
Worsening Symptoms Reveal HS After Misdiagnosis
42-year-old female
Presentation
Patient Description
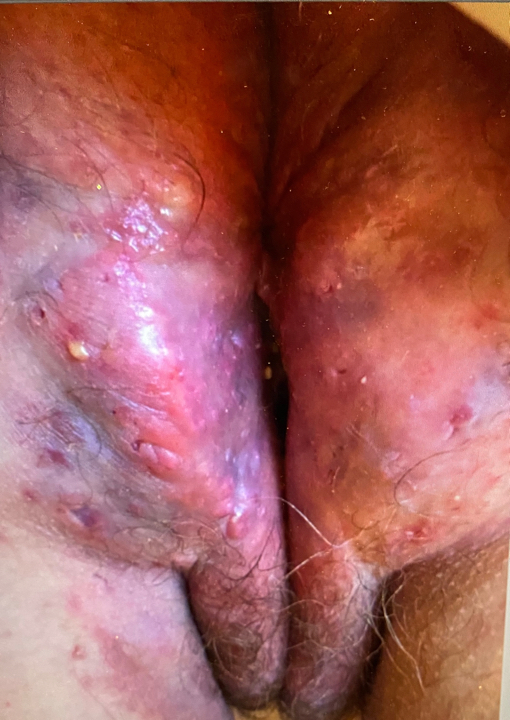
- Patient is a 42-year-old nonobese female who is married and works as a medical secretary. She has a 3-year history of intermittent draining boils and nodules in the genital and buttock areas. Areas of involvement had previously improved with episodic antibiotic management
- Patient now reports worsening redness, drainage, pain, and difficulty sitting. Flares are more frequent, more widespread, and with more severe pain. Flares now occasionally involve new areas (axilla) and are less responsive to antibiotics
- Patient reports significant emotional impact including lack of intimacy with husband and feelings of embarrassment and blame. She uses a donut pillow at work, cannot sit for longer than 30 minutes during flares, and is unable to exercise due to pain
- Patient was seen 10 days prior by her PCP who prescribed a systemic antibiotic for “boils”; limited improvement
- Current medications include an angiotensin receptor blocker for hypertension and a topical corticosteroid for psoriasis
- Preexisting conditions include anemia and nonmelanoma skin cancer (squamous cell carcinoma) of thumb and nose
CASE STUDY 2:
Prompt HS Diagnosis Upon Revealing Symptoms1
22-year-old female
Presentation
Patient Description
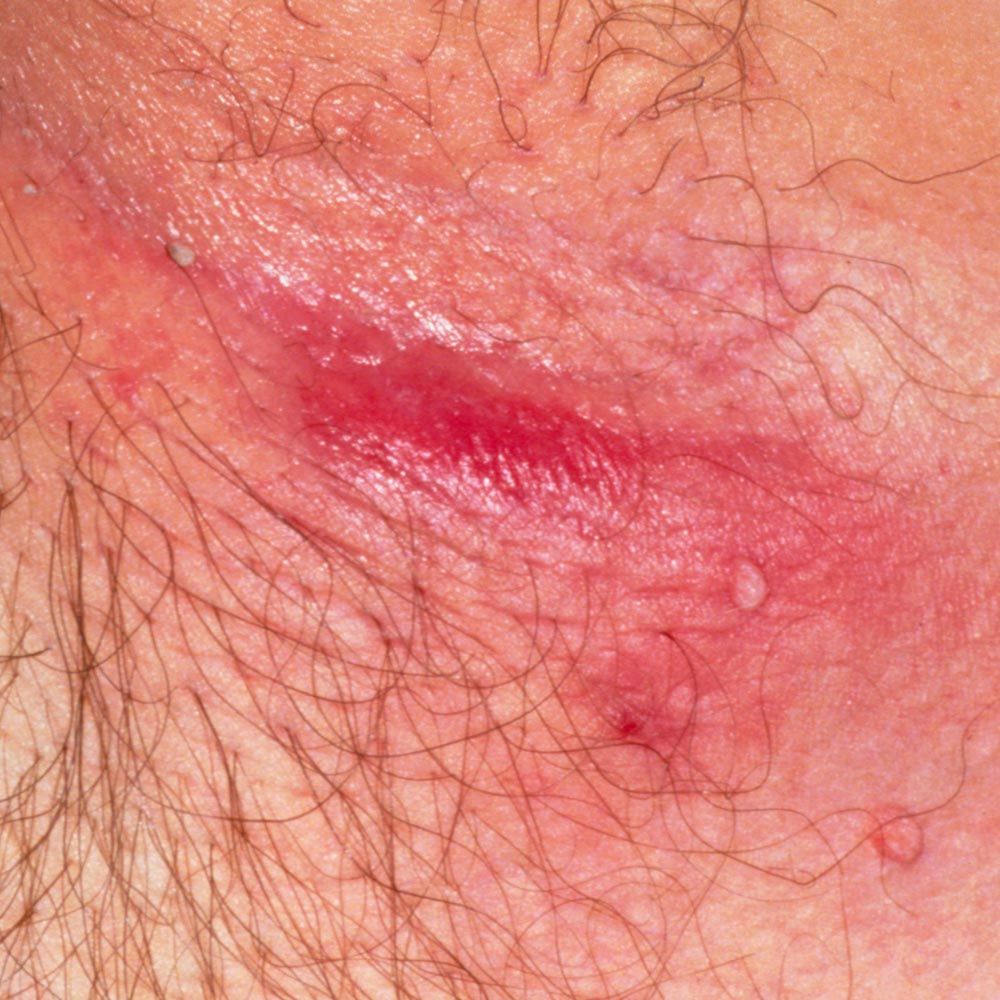
- Patient is a 22-year-old, slightly overweight female. Her marital and job status are unknown. She reported recurring lesions in armpits, under breasts, and groin. She has been managing the condition with obsessive hygiene and cleanliness and has not sought treatment until now. She is not on any medications
- Patient reported feelings of depression, shame, and self-blame, and she noted that the condition has had a negative impact on her relationship
- Patient’s PCP was her OB/GYN, who suspected HS and referred the patient to a dermatologist for diagnosis and treatment
CASE STUDY 3:
Determining HS Management After Misdiagnosis
45-year-old female
Presentation
Patient Description
- Patient is a 45-year-old white female (BMI 24 kg/m2) who is single and works as a finance professional. She has a history of inflammatory lesions in the perianal area and medial thighs since she was a teenager. The initial diagnosis was endometriosis, but was corrected to HS just 1-year prior to this appointment
- Previous medications include an oral cephalosporin antibiotic and an oral contraceptive, and patient is currently taking an oral tetracycline antibiotic
- Patient now reports her lesions are constantly draining fluid, and once to twice per month she develops severely painful abscesses that persist for approximately one week. The abscesses commonly appear during her last week of menses
- Patient communicates a sense of hopelessness due to her long history with the condition and initial misdiagnosis
HS Treatment Options
There are important considerations when developing a multi-modal management plan.2
Co-managing HS With a Specialist
Partner with an experienced HS specialist in dermatology to co-manage your HS patients.
REFERENCES
1. Case study - Hidradenitis suppurativa. GPonline. Published October 25, 2013. Accessed January 29, 2020. https://www.gponline.com/case-study-hidradenitis-suppurativa/dermatology/article/1217733. 2. Lockwood SJ, Prens LM, Porter ML, Kimball AB. Treatment of hidradenitis suppurativa. In: Kimball AB, Jemec GBE, eds. Hidradenitis Suppurativa: A Disease Primer. Switzerland: Springer International Publishing AG; 2017:39-51.