Clinical Presentation of HS
Physical Signs and Symptoms of HS
Hidradenitis suppurativa (HS) is characterized by painful inflamed lesions—nodules or abscesses—that typically manifest in the axillary, inguinal, inframammary, and anogenital regions of the body. Lesions in these locations make HS especially burdensome, impairing sexual health and causing extreme pain and discomfort.1-3
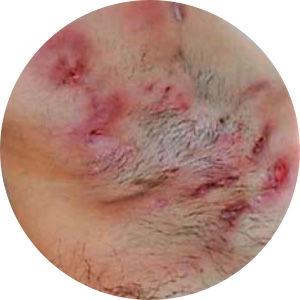
Axillary Abscesses
Lesions in early stages of HS may look similar to those of other skin conditions and of infectious conditions, which can lead to misdiagnosis.4
As the disease progresses, these lesions have a malodorous discharge, and this discharge may require the use of—and frequent changing of—bandages or dressings.2
Without medical intervention, HS may progress to sinus tract formation and permanent scarring, which can limit mobility and be disabling for patients. When the disease has advanced to these later stages, surgery may be needed to remove sinus tracts and scarring.2,5
Location of Symptoms in Female vs Male Patients
View common locations where HS lesions appear.6,7 Click on the hotspots below to show more information.

Axillae
Breast
Groin
Perianal
Female

Nuchal Scalp, Ears
Axillae
Groin
Perianal
Male
Although HS commonly affects these areas, HS lesions can appear anywhere on the body.
By the Numbers: the Impact of HS
In a prospective multinational survey conducted in patients with HS8:
61%
of patients rated their HS-related pain as moderate or higher
53%
of patients experienced flares at least weekly
43%
of patients reported an extreme impact on quality of life
Psychosocial Impact of HS
HS lesions are associated with unsightly lesions, unendurable pain and malodorous discharge, and as a result, patients may experience psychological stress and social stigma.9
The impact of HS on quality of life is more severe than with many other dermatological conditions.9
HS can cause challenges with9:
- Employment
- Depression
- Anxiety
- Loneliness
- Self-esteem
- Sexual impairment
From a Spanish survey of 242 patients with HS10:
27
lost workdays in the last year due to HS
87%
reported HS affecting their daily lives
72%
were unsatisfied or not at all satisfied with their healthcare related to HS
“My HS patient had a hard time sitting due to pain and discomfort of abscesses on her buttocks. She was interviewing for a new job and found it embarrassing and difficult to sit during her interviews. She had been unable to travel anywhere.”
- Primary care physician
HS Diagnosis Quiz
View photos of common differential diagnoses and take the HS diagnosis quiz.
Co-managing HS With a Specialist
Partner with an experienced HS specialist in dermatology to co-manage your HS patients.
REFERENCES
1. Zouboulis CC, Del Marmol V, Mrowietz U, Prens EP, Tzellos T, Jemec GBE. Hidradenitis suppurativa/acne inversa: criteria for diagnosis, severity assessment, classification and disease evaluation. Dermatology. 2015;231(2):184-190. 2. Alikhan A, Lynch PJ, Eisen DB. Hidradenitis suppurativa: a comprehensive review. J Am Acad Dermatol. 2009;60(4):539-561. 3. Shah N. Hidradenitis suppurativa: a treatment challenge. Am Fam Physician. 2005;72(8):1547-1552. 4. Lockwood SJ, Kimball AB. Diagnostic workup. In: Kimball AB, Jemec GBE, eds. Hidradenitis Suppurativa: A Disease Primer. Switzerland: Springer International Publishing AG; 2017:27-37. 5. Jemec GBE. Hidradenitis suppurativa. N Engl J Med. 2012;366(2):158-164. 6. Micheletti RG. Natural history, presentation, and diagnosis of hidradenitis suppurativa. Semin Cutan Med Surg. 2014;33(suppl 3):S51-S53. 7. Vazquez BG, Alikhan A, Weaver AL, Wetter DA, Davis MD. Incidence of hidradenitis suppurativa and associated factors: a population-based study of Olmsted County, Minnesota. J Invest Dermatol. 2013;133(1):97-103. 8. Garg A, Neuren E, Cha D, et al. Evaluating patients' unmet needs in hidradenitis suppurativa: results from the Global Survey Of Impact and Healthcare Needs (VOICE) Project. J Am Acad Dermatol. 2020;82(2):366-376. 9. Kouris A, Platsidaki E, Christodoulou C, et al. Quality of life and psychosocial implications in patients with hidradenitis suppurativa. Dermatology. 2016;232(6):687-691. 10. Strategic health initiative to determine the standard of care: for patients with hidradenitis suppurativa. Sociedad Española de Medicina de la Adolescencia SEMA. Accessed June 9, 2020. https://www.adolescenciasema.org/ficheros/HERCULES%20Informe/Informe%20Hercules%20ENG%205-06-17.pdf.
